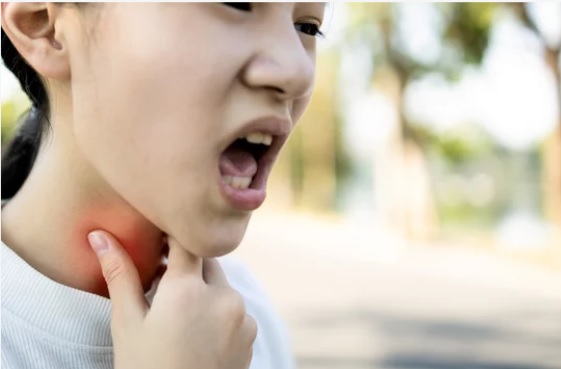
Hoarseness is any change in voice quality from harsh, rough, or raspy voice to weak voice.
It is caused by laryngeal dysfunction.
The vocal cords that are responsible for the voice are part of your voice box (larynx) located in the throat.
When the vocal cords become inflamed or infected, it can cause hoarseness.
The most common cause of hoarseness is a cold or throat infection, which most often goes away on its own within 2 weeks.
A serious cause of hoarseness that does not go away in a few weeks is cancer of the voice box.
What is DYSPHONIA?
Dysphonia, an all-encompassing term, includes any change in voice, increased vocal effort, fatigue, or pain/discomfort with vocal use.
What is APHONIA?
Aphonia means no voice or just whispering.
Etiology of Hoarseness of Voice –
Hoarseness is a symptom and not a disease.
The conditions that interfere with the functions and structure of vocal cords include the following:
Inappropriate approximation: Vocal cord paralysis or fixation, tumors of vocal cords.
Abnormal size: edema or tumor of the vocal cord, partial surgical excision, or fibrosis.
Abnormal stiffness: decrease in paralysis, increase in spastic dysphonia or fibrosis.
Improper vibrations: Congestion, submucosal hemorrhages, nodule, or a polyp.
Types of Voice–
- ROUGH VOICE (vocal cord margin pathology),
- BREATHY VOICE (vocal cord paresis/palsy),
- TIGHTNESS or PAIN in the TONGUE or STRAP MUSCLES (muscle tension dysphonia).
Causes of Hoarseness of Voice–
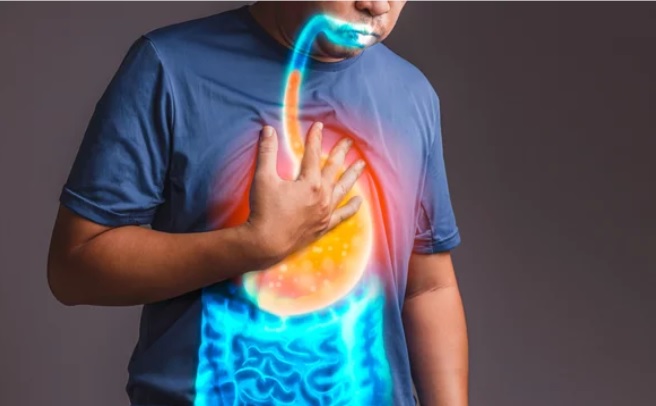
1) Acid reflux (Gastroesophageal or Laryngopharyngeal reflux aka GERD/LPR)
2) Allergies (sneezing, itching, watery eyes)

3) Breathing in irritating substances

4) Cancer of the throat or larynx
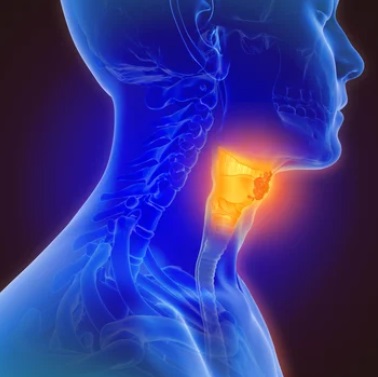
5) Chronic cough

6) Upper respiratory infections

7) Occupation and habits:
Professional voice users like teachers and singers, shouting, irregular and junk food, smoking, and drinking.



Less common causes of hoarseness of voice include:
1) Instrumentation Injury or irritation from a breathing tube or bronchoscopy
2) Foreign object in the esophagus or trachea
3) Damage to the nerves and muscles around the voice box (from trauma or surgery)
4) Ingestion of a harsh chemical liquid
5) During puberty changes in the larynx
6) Thyroid or lung cancer
7) Hypothyroidism
8) Immobility of one or both vocal cords
Home Care
Hoarseness may be acute or chronic.
VOICE REST and time may improve hoarseness.
Hoarseness that does not go away for weeks or months should be checked by a healthcare provider.
Things you can do at home to help relieve the problem include:
1) Keep yourself from using your voice for too long.

2) DO NOT GARGLE AT ALL.

3) Drink plenty of water to help keep your airways moist.

4) Use a humidifier to add moisture to the air you breathe.

5) Avoid actions such as whispering, shouting, crying, and singing as they strain vocal cords.

6) Take an antacid that neutralizes stomach acid if hoarseness is due to gastroesophageal reflux disease (GERD).

7) DO NOT use decongestants WITHOUT ENT DOCTOR’S ADVICE as they can dry out the vocal cords.
8) Stop smoking or cut down at least until hoarseness goes away.

When to Contact an ENT Specialist?
If your voice is still hoarse after three weeks, you should see your healthcare provider. You should see a healthcare provider before then if you have any of the following:
- Difficulty in breathing.
- Pain while speaking.
- Pain while swallowing.
- Coughing up blood.
- Difficulty in swallowing.
- A lump in your neck.
- Hoarseness occurs with drooling, particularly in a small child.
- Hoarseness occurs in a child less than 3 months old.
- Hoarseness has lasted for more than 1 week in a child, or 2 to 3 weeks in an adult.
How is hoarseness diagnosed?
The healthcare provider will examine your throat, neck, and mouth and ask you some questions about your symptoms and medical history.
These may include:
- To what extent have you lost your voice (all or partially)?
- What kind of vocal problems are you having (making scratchy, breathy, or husky vocal sounds)?
- When did hoarseness start?
- Does hoarseness come and go or get worse over time?
- Have you been shouting, singing, or overusing your voice, or crying a lot (if a child)?
- Have you been exposed to harsh fumes or liquids?
- Do you have allergies or a post-nasal drip?
- Have you ever had throat surgery?
- Do you smoke or use alcohol?
- Do you have other symptoms such as fever, cough, sore throat, difficulty swallowing, weight loss, or fatigue?
Most patients can be managed by their general practitioners, but non-responsive patients require an ENT SPECIALIST’S MANAGEMENT.
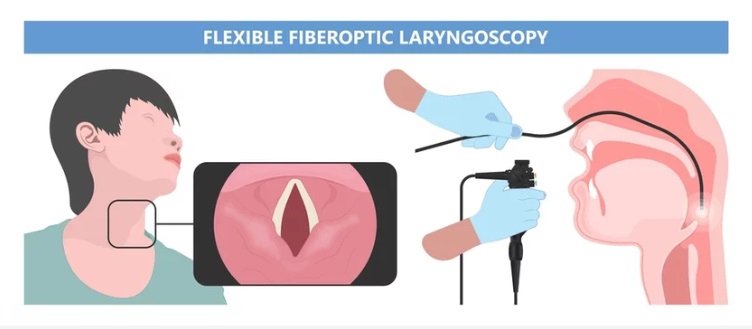
THROAT or LARYNGEAL ENDOSCOPY aka Flexible Fiberoptic Laryngoscopy, an OPD procedure can easily show congestion, edema, polyp, nodule, or growth if present over the vocal cord.
THANK YOU
MEDICAL ADVICE DISCLAIMER:
This blog including information, content, references, and opinions is for informational purposes only.
The Author does not provide any medical advice on this platform.
Viewing, accessing, or reading this blog does not establish any doctor-patient relationship.
The information provided in this blog does not replace the services and opinions of a qualified medical professional who examines you and then prescribes medicines.
And if you have any questions of medical nature, please refer to your doctor or qualified medical personnel for evaluation and management at a clinic/hospital near you.
The content provided in this blog represents the Author’s own interpretation of research articles.