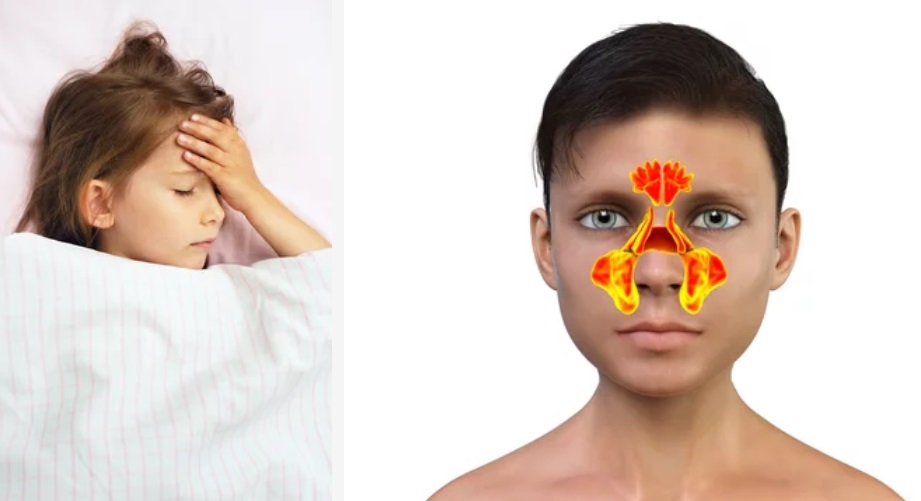
Pediatric Rhinosinusitis (RS) is a multifactorial disease, and the importance of the predisposing factors changes with increasing age.
Depending on the course of the disease, it is divided into —
- Acute (10 days to < 3 weeks),
- Subacute (3 weeks to < 12 weeks), and
- Chronic (> 12 weeks).
In recurrent disease, complete resolution occurs between the episodes, which are 3 or more in 6 months or more than 4 in 1 year.
Pathophysiology
1. Obstruction in the drainage pathways of the sinuses results in stasis of secretions that lead to sinus disease. The obstruction may be anatomic, physiologic, or both.
2. The anatomic obstruction can be due to turbinate (hypertrophic or enlarged, concha bullosa or pneumatized and paradoxical bend), septum (deviation and spur), polyps, enlarged adenoids and mucosal inflammation from allergy, infection, and irritation.
3. Other conditions which may increase the incidence of sinus disease includes allergy, GERD, air pollution, first- or second-hand smoke and daycare environment.
Clinical Features
ACUTE RHINOSINUSITIS
It is often preceded by viral upper respiratory infection (URI) with clear nasal discharge, which often recedes within 5 days.
If the symptoms of purulent discharge, facial pain, nasal obstruction, and daytime cough persist longer than 10 days, a diagnosis of acute sinusitis should be considered.
The features of severe infection include high fever (> 40°C) and periorbital edema.
CHRONIC RHINOSINUSITIS
Clinical features include night time cough, nasal discharge and obstruction, and postnasal drip. Headache wax and wane symptoms persist for more than 12 weeks.
Other features include facial pain, ocular or dental pain, sore throat, low-grade fever, and asthma.
Differential Diagnosis
- Allergic rhinitis
- Recalcitrant rhinosinusitis: Consider and evaluate for immunodeficiency, cystic fibrosis, ciliary immotility disorders, and GERD.
Diagnosis of Pediatric Rhinosinusitis
1. Clinical — All the symptoms mentioned in the clinical features section need to be looked for
2. Nasal endoscopic examination — to look for DNS, hypertrophied turbinate, a nasal mass, Pus, or secretions in the sinuses.
3. Culture of sinus secretions.
4. Allergic assessment: Skin prick test, nasal smear, RAST, and trial of treatment.
5. CT scan of the Paranasal Sinuses (PNS): Though the gold standard for evaluating sinonasal disease, CT is not necessary to confirm the diagnosis of rhinosinusitis in children. It is indicated only when sinus surgery is considered.
Treatment of Pediatric Rhinosinusitis
1. Medical therapy: It is the initial treatment modality.
Antibiotics, which are indicated in following children, allow for earlier resolution and may prevent complications.
– Severe acute RS
– Acute RS with the protracted course.
– Suspected or proven suppurative complications
a. Acute rhinosinusitis: Antibiotics for 10–14 days; prolonged to 1 month when symptoms do not resolve completely.
– First line antibiotic: Amoxicillin at the normal or high dose.
– First line alternatives (Children allergic to penicillin): Cefdinir, cefuroxime, cefpodoxime, azithromycin (for 3 days) or clarithromycin.
– Second line antibiotics (unresponsive, more severe disease or resistant S. pneumoniae): High-dose amoxicillin/clavulanate (90 mg/kg amoxicillin).
– Children with vomiting: Parenteral ceftriaxone.
b. Chronic rhinosinusitis:
– Beta lactam stable antibiotic for 3 weeks
– Topical nasal sprays:
- Saline nasal sprays for children under 2 years
- Fluticasone propionate for children 4 years and beyond
- Mometasone furoate for children 6 years and beyond
– Antihistamines: Newer nonsedating
– Mucolytics: Guaifenesin
2. Surgical treatment: It is rarely needed except in cases of orbital or intracranial complications.
a. Adenoidectomy: In the presence of adenoid hypertrophy in cases of chronic rhinosinusitis (CRS).
b. Functional endoscopic sinus surgery: in cases of orbital or intracranial complications.
THANK YOU
MEDICAL ADVICE DISCLAIMER:
This blog including information, content, references, and opinions is for informational purposes only.
The Author does not provide any medical advice on this platform.
Viewing, accessing, or reading this blog does not establish any doctor-patient relationship.
The information provided in this blog does not replace the services and opinions of a qualified medical professional who examines you and then prescribes medicines.
And if you have any questions of medical nature, please refer to your doctor or qualified medical personnel for evaluation and management at a clinic/hospital near you.
The content provided in this blog represents the Author’s own interpretation of research articles.