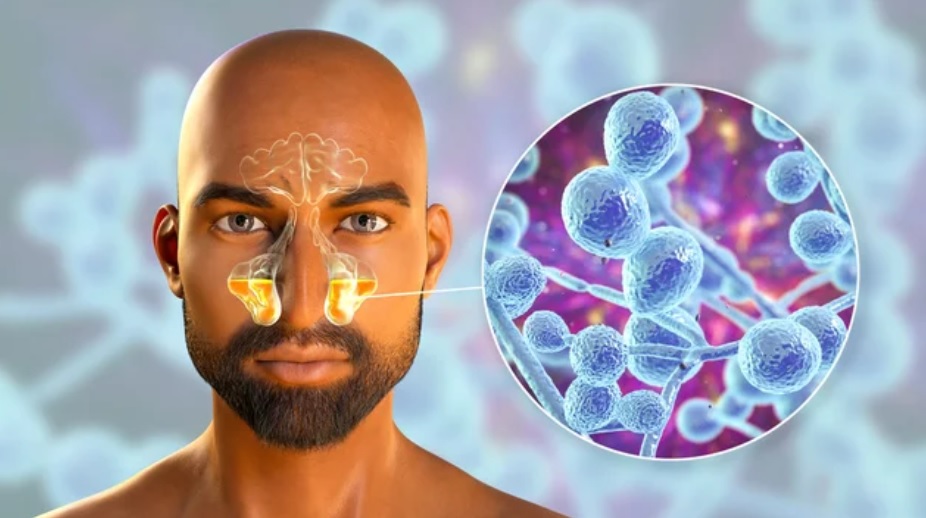
Definition:
FUNGAL SINUSITIS is inflammation of paranasal sinuses caused by fungal infection.
It is a broad term used to describe various conditions when fungus may involved in the cause or symptoms of nasal and sinus inflammation.
It usually occurs in immunocompromised people.
Fungal rhinosinusitis encompasses a wide variety of fungal infections that range from merely irritating to rapidly fatal.
TYPES OF FUNGAL SINUSITIS —
Fungal rhinosinusitis has 5 distinct forms:
1. Noninvasive
– Fungus Balls
– Saprophytic Fungal Infection
– Allergic Fungal Rhinosinusitis
2. Invasive
– Acute Invasive Fungal Sinusitis
– Chronic Invasive Fungal Sinusitis
Why is Immunology Important in Fungal Sinusitis?
The evaluation of the immunologic status of the patient is very important because fungal sinusitis is related to host immunocompetency.
Clinical features of FUNGAL SINUSITIS:
The chronic symptoms in NON-INVASIVE FUNGAL SINUSITIS include —
- Facial pain,
- Nasal obstruction,
- Cacosmia (means altered sense of smell or unpleasant smell sensation)
- Nasal polyps,
- Proptosis (Protrusion or eyeball or Outbulging of eyeball)
- Allergic mucin casts.
Allergic Fungal Rhinosinusitis
The manifestations of this noninvasive fungus occur because of a hypersensitivity response by the patient to the fungus.
Etiology—
Dematiaceous (darkly pigmented) fungal species include Alternaria, Bipolaris, and Curvularia.
Clinical features —
Allergic fungal rhinosinusitis (AFRS) is found in cases of allergy, polyps, and allergic mucin nasal casts.
Laboratory —-
a) Eosinophilia.
b) Total immunoglobulin IgE is raised along with fungus specific IgE and IgG, which are difficult to evaluate as many fungi cause AFRS.
c) In quiescent AFRS, total IgE may be normal.
CT scan —
AFRS shows heterogeneity of tissue densities within the sinuses. Post contrast MRI shows fungal growth with changes of sinusitis.
Histopathology —
Hyphae are seen in eosinophil-rich mucin without any evidence of tissue invasion. So the pathologist should assess the mucin, not the polyp.
Allergic mucin contains necrotic inflammatory cells, eosinophils, and Charcot-Leyden crystals (a byproduct of eosinophil degranulation).
Treatment —
It includes surgery, steroids, immunotherapy, and antifungal agents.
Surgery —
Surgical removal of all allergic mucin.
- Steroids: If it is difficult to remove allergic mucin completely, then remission is achieved with systemic steroids.
- In cases of recurrence, repeated surgical removal of mucin combined with perioperative steroids (prednisolone 60 mg for several days and tapered off over 2 to 4 weeks) is beneficial.
- Immunotherapy: It contains fungal agents, starts within 4–8 weeks of surgery, and prevents recurrence.
- Oral antifungal agents: Their role is controversial. A long course of oral itraconazole (400 mg daily for 1 month and tapered over 3 months) needs regular monitoring of liver functions. It has shown good results.
Fungus Balls
a. Causative fungal species: The fungi presenting with balls are A. flavus, A. fumigatus, Alternaria and Mucor.
b. Sites: Maxillary sinus is most commonly involved followed in descending frequency by sphenoid, ethmoid and the frontal.
c. Clinical features: This noninvasive fungus may remain asymptomatic for months to years but may become invasive if the patient becomes immunocompromised.
- It may present with facial pain and cacosmia.
d. CT scan: Fungus balls show total or partial sinus opacification (hyperdense area) and rarely bony erosion.
e. Diagnosis: It is usually diagnosed at surgery and suspected on CT scans.
- Culture may be negative but fungus can be seen with special stains.
f. Treatment: Usually no antifungal therapy is required. The recurrence after surgical removal is uncommon.
Saprophytic Fungal Infection
- Clinical: The fungus grows on mucocrusts, seen after endoscopic sinus surgery (ESS).
- Treatment: It includes removal of crusts.
- Prevention: The patient is instructed to irrigate the nose weekly with sterile saline and wear a mask in moldy environments.
Acute Invasive Fungal Sinusitis
Etiology of Acute Invasive Fungal Sinusitis:
The most common fungi are —
Aspergillus species,
Mucorales (mucormycosis).
Mucormycosis:
It is more common in diabetics.
Fungal elements are broad, ribbon-like (10–15 mm), irregular and rarely septated.
Aspergillus:
This species have narrow hyphae with regular septations and 45° branching.
Clinical features of Acute Invasive Fungal Sinusitis:
The immunocompromised patients (Diabetic, Transplant, Leukemia, and AIDS) are most at risk for invasive fungus.
These cases need quick evaluation and aggressive management.
Steroids administration may be one of the precipitating factors.
a. Acute clinical picture: It includes palatal erosion, impairment of vision, limitations in extraocular movements, fever, nasal and facial anesthesia and nasal necrosis.
b. Mucopurulence: It is variable depending on the neutropenia of the host.
Investigations: The investigations are as follows:
a. CBC in immunosuppressed patients may show neutropenia or evidence of left shift.
b. Coagulation profile includes platelets, bleeding time, prothrombin time and partial thromboplastin time.
c. Blood sugar is found raised in invasive fungus especially mucormycosis.
d. In culture an endoscopic aspirate culture is done with immediate fungal stains.
e. In biopsy if fungal stains are negative and suspicion is strong then biopsy with immediate frozen section and fungal stains are done. Coagulation abnormalities if any are corrected before biopsy.
f. CEMRI scan of Paranasal sinuses, Orbit, and Brain: It is the most important radiological modality now-a-days in cases of mucormycosis as it not only tells us about the spread of the fingus but also helps ion planning the fungal sinus surgery.
– Axial scans provide additional information for the funguses of frontal and sphenoidal sinuses. Contrast studies are ordered if invasive fungus shows bony erosion, intracranial or orbital extension.
Treatment:
Attempts must be made to reverse the immunocompromised status by controlling its cause.
a. Conservative debridement:
Repeated conservative debridement (removal of necrotic tissue) may be needed in operative candidates, whose immunocompromised state can be reversed.
Orbital exenteration should be avoided, when patient is not blind, even if there is involvement of the orbit. In cases of bone marrow transplant, when ingraft fails, immunocompromised state cannot be reversed and heroic surgeries are futile and must not be done.
b. Antifungal agents:
The systemic and topical antifungal agents appropriate for the cultured fungus must be started immediately.
– Intravenous amphotericin B is usually started while awaiting fungal report.
– Itraconazole: If Pseudallescheria boydii grows on culture.
How to prevent the Fungal Infection ?
The use of high-efficiency particulate air filter systems and elimination of potted plants can reduce fungal infection in high-risk neutropenic patients.
Chronic Invasive Fungal Sinusitis
- Causative fungi: Aspergillus flavus (most common), Aspergillus fumigatus, Alternaria, P. boydii, Sporothrix schenckii.
- Types: There are two types of chronic indolent invasive fungal sinusitis and both progress over weeks to months to years.
a. Granulomatous: It is common in Sudan and infects immunocompetent patients.
b. Nongranulomatous: It occurs in immunocompromised patients.
- Diagnosis: Fungal culture and biopsy with special fungus stains confirm the diagnosis.
- Treatment: It consists of–
- Repeated courses of antifungal therapy.
- Surgical debridement.
- Attempts to control the cause of immunocompromise.
THANK YOU
MEDICAL ADVICE DISCLAIMER:
This blog including information, content, references, and opinions is for informational purposes only.
The Author does not provide any medical advice on this platform.
Viewing, accessing, or reading this blog does not establish any doctor-patient relationship.
The information provided in this blog does not replace the services and opinions of a qualified medical professional who examines you and then prescribes medicines.
And if you have any questions of medical nature, please refer to your doctor or qualified medical personnel for evaluation and management at a clinic/hospital near you.
The content provided in this blog represents the Author’s own interpretation of research articles.