According to new reports, a new disease called Monkeypox is jumping from one country to another.
Now you think, what’s that?
Well, Monkeypox is not new but an old virus that has resurfaced. Well, to know what it can do and what not, let us explore more about this condition.
The coronavirus pandemic has shown us just how quickly a virus can wreak havoc on society in just the span of two years. So much has changed as a result of COVID-19, and many people are fearful that we may experience another COVID-level pandemic in the near future. Recently, there has been a lot of talk about Monkeypox and a potential outbreak, but…
what is Monkeypox, how serious is it, and should you be concerned, let’s talk about it.
The world is still reeling from COVID-19, and now we have a new health crisis to deal with. The WHO declared Monkeypox a global health emergency. They say more than 16000 cases have been confirmed so far in 75 countries. There are 4 known Monkeypox cases in India till July 2022. Several states have now been deploying strict screening protocols, and the center has asked officials to remain on alert.
According to the WHO, Monkeypox is a virus with symptoms very similar to those seen in the past in smallpox patients, although it is clinically less severe. Thankfully, fatality rates in this are low.
The WHO goes on to say that uncertainty remains on the natural history of the Monkeypox virus, and further studies are needed to identify the exact reservoirs and how virus circulation is maintained in nature.
The chief scientist at the WHO has said that the outbreak of Monkeypox has been a wake-up call and explained that since 1980 or so, smallpox vaccination programs have been stopped indicating that may have helped the virus to steal a march on the world.
The WHO website says that vaccines used during the smallpox eradication program also provide protection against Monkeypox, but newer vaccines have been developed as well, of which one has been approved for the prevention of Monkeypox.
Using the smallpox vaccine for Monkeypox may be useful, though more laboratory data is required. There is a Denmark-based company called Bavarian Nordic that has developed a vaccine for Monkeypox, but there isn’t any efficacy data on that yet. Indian pharmaceutical companies like the Serum Institute of India can have a big role in bottling, marketing, and distributing existing smallpox vaccines if they are widely available.
What is Monkeypox?
Monkeypox is a disease caused by infection with the Monkeypox virus. It belongs to the family of viruses known as the Orthopoxvirus genus of the Poxviridae family, which also includes things like Smallpox, Vaccinia, and Cowpox.
Monkeypox was first discovered in 1958 when 2 outbreaks of a pox-like disease emerged in a group of monkeys kept for research, hence it was named Monkeypox. Later in the 1970s, when it started to infect people of Central and Western Africa, scientists found out that it is a zoonotic disease meaning a disease that transmits from animals to humans.
It is caused by a virus belonging to the Orthopoxvirus genus that has an oval-shaped appearance. It also comes from the same family of viruses known to spread smallpox and cowpox. Though they were first found in monkeys, however, these microbes can also be found in other animals, especially rodents.
What are the signs and symptoms of Monkeypox?
According to the US Center for Disease Control and Prevention, the main symptoms are:
1) Fever
2) Headache
3) Muscle aches
4) Backache
5) Swollen lymph nodes
6) Chills
7) Exhaustion
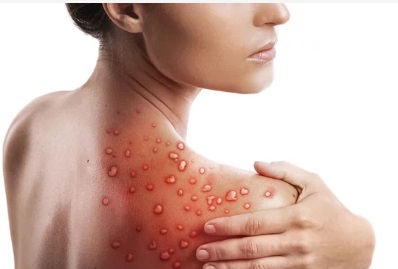
8) Rash or Painful lesions on the whole body
Importantly, a rash can look like pimples or blisters that appear on the face, inside the mouth, and on other parts of the body like your hands, feet, chest, etc. The rash goes through different stages before it heals completely. Sometimes people get a rash first, followed by other symptoms. Others only experience a rash.
9) Sore throat
10) Cough
11) Lack of energy
Diagnosis of Monkeypox infection:
Polymerase chain reaction (PCR) is the preferred laboratory test for the diagnosis of Monkeypox.
If Monkeypox is suspected, the healthcare provider will collect a lesion sample and transport it safely to a laboratory with appropriate capability.
Optimal diagnostic samples for Monkeypox are from—
a) Skin lesions,
b) the roof or fluid from vesicles, and
c) Pustules and dry crusts.
A blood sample may also be needed to check for the Monkeypox virus.
What can we do to protect ourselves from Monkeypox infection?
Fortunately, Monkeypox is usually mild, and most people recover within a few weeks, but as the infection can spread through close contact and can get severe, it’s essential to isolate if someone is suffering from it.
And for others, make sure to avoid contact with any materials such as bedding or clothing that have been in contact with a sick human or animal.
- Avoid close contact with people who have suspected or confirmed Monkeypox.
- Isolate infected patients from others.
- Practice good hand hygiene. Clean hands regularly with soap and water or alcohol-based hand rub.
- Use appropriate personal protective equipment (PPE) when caring for patients.
- Wear a medical mask and advice the patient to wear one and advise on Respiratory Hygiene and Cough Etiquette.
- Avoid skin-to-skin contact and use disposable gloves.
- Make sure to cook your food properly.
Monitoring and Treatment of Complications:
The patient should be closely monitored for the appearance of any of the following symptoms during the period of isolation–
- Pain in the eye or blurring of vision.
- Shortness of breath.
- Chest pain.
- Difficulty in breathing.
- Altered consciousness.
- Seizure.
- Decrease in urine output.
- Poor oral intake.
- Lethargy.
In case any of the above symptoms appear, the patient should immediately contact a nearby healthcare facility/specialist.
How do humans get the infection?
Well, Animal-to-Human transmission can occur from direct contact with infected animals’ blood, bodily fluids, or mucosal lesions.
Also, eating undercooked meat of infected animals can contribute to catching this infection.
So, once infection happens, in a couple of weeks or so, the person starts to get flu-like symptoms like fever, chills, muscle pain and headaches, fatigue, as well as swollen lymph nodes.
Then within 1 to 3 days of getting a fever, skin eruptions start to occur, and the patient gets fluid-filled bumps, mostly on the face, followed by palms and soles of the feet that could last around 2 to 4 weeks before it starts to go away.
And if such a person does not isolate and comes in contact with others during the infection phase, he or she can spread it amongst others. This could be a possible reason for this disease being found in other countries around the world today.
Why has Monkeypox re-emerged?
Researchers are still trying to figure it out, but one possible reason could be eradicating smallpox from the world.
Yes, that’s because smallpox was on the rage nearly 40 years ago, so it was a kind of compulsion to take smallpox vaccines to prevent it, and as smallpox and Monkeypox viruses belong to the same family, the vaccines also protected against Monkeypox infection. But since the extinction of smallpox, the new generation no longer needs these vaccines. So this could have given the Monkeypox virus another chance to infect unvaccinated people.
Human Monkeypox was first identified in humans in 1970 in the Democratic Republic of the Congo in a 9-month-old boy. In 2003, 47 confirmed and probable cases of Monkeypox were reported in six states of the USA due to people coming in touch with imported pet prairie dogs.
What are the variants of Monkeypox?
There are 2 main variants of the Monkeypox virus —
– The Congo Basin clade, and
– the Central Africa clade.
The congo basin variant has historically caused more severe disease and is thought to be more transmissible regardless Monkeypox is much less transmissible than smallpox, and the symptoms tend to be much milder, much like other viral illnesses.
The first 1 to 3 days are characterized by fever, chills, fatigue, headaches, muscle ache, and swollen lymph nodes, after which infected individuals will start developing a rash that progresses from small flat lesions to eventually large fluid-filled blisters. Over the span of the next few weeks, these blisters will drain, scab over, and eventually fall off. The disease is usually self-limiting, meaning that it usually goes away on its own and generally lasts anywhere from 2 to 4 weeks before subsiding that being said, some individuals experience much more severe symptoms and develop more dangerous issues such as secondary infection, sepsis, and pneumonia to name a few. As many as 1 in 10 people who become infected with Monkeypox in Africa die from the disease.
If we have known about Monkeypox for over 50 years, why are we so concerned about it now?
The reason is that as of May 2022, dozens of cases have begun to appear outside of Africa, where the virus has largely been contained for decades.
This is concerning because the primary mode of transmission from Monkeypox has been from animal to human, such as from a rat. The individual may go on to infect a close family member or two, but historically the disease has fizzled out quickly. But now, human-to-human transmission is rising.
Human-to-human transmission is thought to occur primarily through direct contact or through large respiratory droplets or contact with body fluids or lesions. As such transmission rates have been relatively low historically and limiting close contact with infected individuals has often been sufficient to prevent the further spread of the disease.
The reason that this current outbreak is causing such a commotion is that the disease is not following its normal pattern of transmission and more people are becoming infected with Monkeypox presumably by human-to-human contact.
Concerns related to Monkeypox:
1. Mortality:
According to the WHO, the case fatality ratio has been estimated to be around 3% to 6%, however, there is an important variable to consider with these numbers in regions of Africa where Monkeypox is more commonly found, and there is often limited access to healthcare.
Often times severe complications from viral illnesses such as secondary infection and sepsis can be treated with supportive care including antipyretics, antibiotics, oxygen, fluids, and close observation. Patients essentially just need a little bit of extra help while their body is recovering from the illness.
In addition, there are also some medications available that can be used to help treat more severe cases of Monkeypox, including the antiviral medications, Tecovirimat and Brincidofovir. For these reasons, the estimated 3 to 6% case fatality ratio may not be representative in countries with greater access to healthcare.
In essence, it is not necessarily the Monkeypox virus alone that is proving fatal but rather having Monkeypox and not having access to supportive care. This is one reason why rising numbers of COVID-19 cases have been so concerning over the past few years. When hospital systems are inundated with patients they don’t have a buffer and access to care can be affected negatively leading people to lose their lives that otherwise wouldn’t have. That being said, even if the case fatality ratio of Monkeypox is less than the estimated 3 to 6%, the case fatality ratio of COVID-19 is estimated between 0.5 and 3%, depending on the country, and we can see how many people have died so should we still be concerned.
2. Mode of Transmission:
The issue with COVID-19 is that it’s very easily transmitted between individuals when an infected person coughs, sneezes, or even just talks, the tiny respiratory droplets carry the virus into the air, and anyone around the individual can then breathe those tiny droplets into their lungs, and they become infected. As a result, coronavirus can spread quickly through a population.
Monkeypox, on the other hand, does not spread that way, transmission from animal-to-human or human-to-human is largely thought to occur through direct contact with large respiratory droplets or body fluids and lesion material.
Monkeypox historically has needed direct physical contact, and some individuals who were infected with Monkeypox in earlier times sometimes didn’t even infect a single person. As a result, the virus did not use to spread efficiently through humans to allow it to sustain itself in the population. This is why the virus has largely remained endemic to Africa, and most cases have occurred due to animal-to-human transmission. Those at risk for human-to-human infection are often close family members or healthcare workers that are treating patients infected with Monkeypox, and even then, much of that risk seems to be largely mitigated with proper contact precautions, but if it’s not so easy to transmit from person to person why do we see so many cases recently, possibly a mutation.
3. Mutation:
The biggest concern is that the virus has changed so that it can be transmitted more easily between humans, and that’s why we see an increased number of cases. According to reports, research is currently being conducted to see if there has been changing to the genome of Monkeypox, however, more research still needs to be done given the type of virus that Monkeypox is however, it is much less likely to mutate than something like COVID-19. The monkeypox virus is a DNA virus.
How does Monkeypox spread?
Monkeypox spreads in different ways. It can spread from —
– person to person,
– through direct contact with the rash itself,
– the scabs,
– the respiratory secretions during prolonged face-to-face contact or
– during intimate physical contacts like kissing, cuddling, or sex.
– Now, touching items such as clothing or linens that previously touched the infectious rash or body fluids can also infect you.
– Pregnant women can spread the virus to the fetus also through the placenta.
– It is also possible for people to get Monkeypox from infected animals, either by being bitten by them or scratched by them or by preparing or eating meat or using products from an infected animal.
What is the treatment for Monkeypox?
There is currently no treatment for Monkeypox, however, this disease is self-limiting, which means it can get better without treatment.
Some medications can be used to prevent the spread of this disease. They include —
– Vaccinia vaccine, which is a smallpox vaccine, and
– VIG (Vaccinia Immune Globulin).
According to the WHO, the smallpox vaccine is approximately 85% effective in preventing the development of the Monkeypox virus. The WHO underlines that it is important not to confuse Monkeypox with chickenpox, measles, bacterial skin infections, scabies, syphilis, and medication-associated allergies.
There are things to keep in mind that we can use for patients with Monkeypox.
- Currently, there are 3 antiviral compounds such as ST-246, Cidofovir, and CMX-001 that are being assessed to treat Monkeypox.
- Monkeypox patients should follow the advice of their health care provider.
- Symptoms normally resolve on their own without the need for treatment.
If needed, medication for pain (analgesics) and fever (antipyretics) can be used to relieve some symptoms. - It is important to stay hydrated for Monkeypox patients.
- The patient should eat well and get enough sleep.
- People who are self-isolating should take care of their mental health by doing things they find relaxing and enjoyable.
- Do exercise if you feel well enough and can do so while isolating.
- Monkeypox patients should avoid scratching their skin and should clean their hands before and after touching lesions and keeping skin dry and uncovered.
- The rash can be kept clean with sterilized water or antiseptic.
- Saltwater rinses can be used for lesions in the mouth.
- Use warm baths with baking soda and Epsom salts for lesions on the body.
- Lidocaine can be applied to oral and perianal lesions to relieve pain.
Conclusion:
Due to these factors, it’s very unlikely that this is going to turn into another COVID-19-like gigantic pandemic. What’s more likely is that it’s going to just fizzle out in the coming months. That being said, it is still important to be aware of Monkeypox, especially if you are in a population that is at higher risk of infection or complications or if you live in an area that is experiencing a lot of cases.
In addition, if you are experiencing fever, body aches, fatigue, swollen lymph nodes, and especially a vesicular rash then you definitely go to see your doctor and get it checked out. Although seeing headlines about Monkeypox and whatever other virus or disease comes next can be scary, you should always try to separate the signal from the noise.
Thank You
MEDICAL ADVICE DISCLAIMER:
This blog, including information, content, references, and opinions, is for informational purposes only.
The Author does not provide any medical advice on this platform.
Viewing, accessing, or reading this blog does not establish any doctor-patient relationship.
The information provided in this blog does not replace the services and opinions of a qualified medical professional who examines you and then prescribes medicines.
And if you have any questions of medical nature, please refer to your doctor or qualified medical personnel for evaluation and management at a clinic/hospital near you.
The content provided in this blog represents the Author’s own interpretation of research articles.